Review best practices for the back office that can help you optimize reimbursement and improve some of your processes such as collections, contract management, denials, claim follow-up and more.
Back-end staff is critical to make sure that you are getting paid for your work. They often deal with many different payers and their guidelines, which makes the upfront verification even more critical. Communication with the back office is key. Their input to the front desk is essential to detect trending issues on your denials and put processes in place to stop or reduce these barriers that prevent you from getting reimbursement.
On the last installment of our Best Practice webinar series, Caroline Balestra, Business Process Analyst at Health Prime, gave an overview of some techniques you can implement in your back office to improve their processes.
Managing payer contracts
Before the visit, Back Office has a responsibility to communicate:
- Specific payer guidelines and payer benefit requirements: helping the front office understand any payer specific guidelines and payer benefit requirements (if necessary) that they need to be aware of when booking patients can help dramatically increase reimbursements.
- Practices and providers payer contracts: One of the primary tasks for back-office personnel is to properly manage these type of contracts, as well as monitor payer reimbursement accuracy and billing performance. If the team takes the time to assess payer performance and payment accuracy, organizations will be able to negotiate better reimbursement rates and improve medical billing compliance.
- Network status for practice and provider: Back-office staff must communicate the network status with the front desk and each of your providers. For example, not doing this could mean that maybe an in-network copayment was collected vs. a larger out of network deductible payment.
- Trend charge capture, rejections and denials: Some practices often employ several staff members to flag charge capture issues and rework the charges. Using a system that trends charge capture data may improve back-end revenue cycle processes. Your HPI optimization team can report on such trends with charge capture, rejections and denials. Being able to trend the data and have a conversation with staff and clinical teams and providers can be helpful in preventing issues going forward.
- Assess and renegotiate as needed: Back-office personnel are usually responsible for negotiating fee schedules with the contracted payers. Understanding how to work with payers to get CPT codes added to your fee schedule or allowable reimbursement amounts increased on those fee schedules is key to best practices where contracts are concerned.
AR & Collections
The complex web of different payer requirements can make claim submission a challenge. As Balestra explained on the second installment of our Best Practices webinar: For the Front Desk, prebilling verification and check-in can help prevent claim issues. However, the back office can assist in getting claims paid as well.
How to prevent claim issues?

As back-end staff collect payments from payers and patients, they complete the healthcare revenue cycle by posting payments to the patient case and closing patient accounts. The front and back end staff handle very different parts of RCM, breaking down the siloes between the two components can improve an organization's financial performance.
Denials & Claims Follow Up
Some of the best practices in working with insurance denials are:
- Quantify the denials: You can't manage what you can't measure. Determine how many denials you have on a specific period of time and what are the reasons behind them.
- Develop a plan to avoid denials: Implement a solid denial management process. Understand the volume of each of your denials, the root cause of each and what the payer will possibly pay, so effective corrections can be made and refilled promptly for your claims.
- Post $0 denials: Ensure that all denials including zero-dollar EOB's are posted. Posting of zero pays will allow for better reporting and denial management.
- Create updated Billing rules: Keep a rules document for any billing rules you need to know about. This way, your entire billing team will function as one. If you work with Health Prime, each account has a practice specific billing rules document. This document is constantly updated to avoid certain denials.
For resubmission and appeals, it is important to follow payer guidelines. Always be sure to:

- Review remittance remarks: check these remarks on an ERA or EOB can be extremely helpful in identifying that the issue is with any claim that has been denied.
- File a corrected claim electronically: Most all primary new claims today are filed electronically. In addition to those, payers will also accept most corrected claims and secondary claims electronically. This makes resubmission to get a corrected claim on file much more timely. Corrected claims should be sent with all line items filled out, not just the line items that need to be corrected. Make sure to use the “original” claim number so the payer knows which claim to replace or void out of their system.
- Submit appeals/reconsiderations online or use payer forms: once you have determined an appeal can be submitted, ensure you are within the timely filing deadlines. Many payers will give you a deadline from the denied date to do this so it's important to pay close attention to the dates or just ask if not sure.
- Know where to send an appeal: Utilize the proper form for reconsideration for applicable and use proper and effective language in those appeals.
- Track appeals: Once your appeal has been submitted its important to follow and track those appeals through to a decision.
Bridge the gap between Front & Back Office
"An efficient communication between your front and back office is essential to run your medical practice effectively. A lack of communication between your team can lead to an ever-widening gap unless is addressed appropriately".
-Balestra explained.
To ensure long-term viability and sustainability, you must address the gap among staff members to improve practice's efficiency, revenue, patient satisfaction and more.
Some tips to improve communications between front and back office are:

Reporting for success
To ensure all the changes you have made to improve your front and back-office processes, you will need the ability to run reports that can help you identify if the implemented changes are having an effect on your metrics.
Our Health Prime Datalytics practice optimization tool can be used to help you in measuring your success with any recent workflow changes within the office. You can view different metrics at a glance, but also dig deep as you need to into each area that can help you identify where your focus might need to be at a given time.
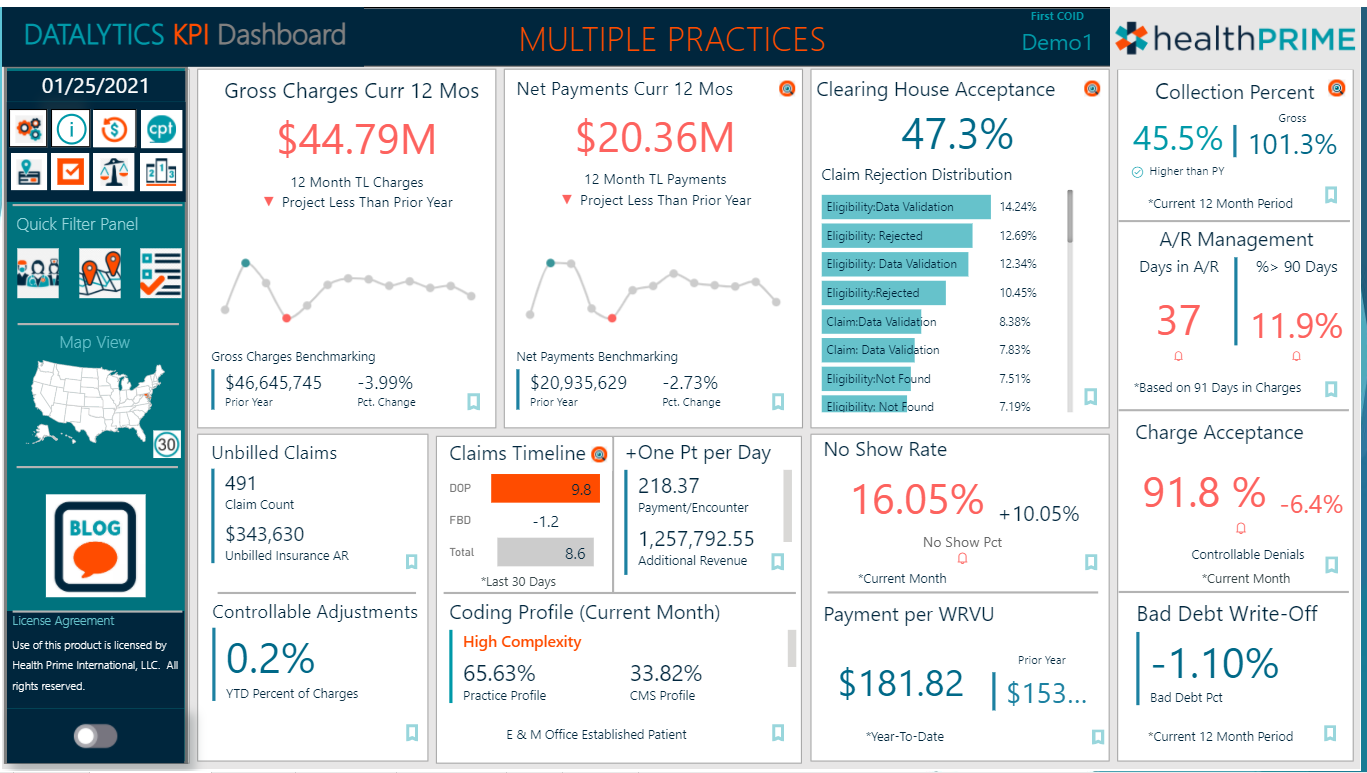
Some focused reports you can pull out from Datalytics are clearinghouse acceptance, net collection rates/collection percent, A/R management, charge acceptance and no-show rates. There are other reports on the Health Prime Datalytics dashboard that you can utilize but these are a few examples.
If you want to know more about Health Prime Datalytics, make sure to follow us on our Datalytics blog. Stay tuned for future articles in the blog series to see how our business intelligence platform has had a tremendous impact in physician practice revenue cycle management.
Partnering with Health Prime
The Healthcare revenue cycle is a complex process of managing revenue as it flows through an organization. Revenue cycle staff from the front and back ends should partner and constantly communicate to ensure revenue flows smoothly.
At Health Prime, we offer partnerships with your practice to optimize your revenue. We have a track record of increasing the average percentage of claims paid after first submission, improved net revenue to the practice, reduced controllable denial rates, improved claim payments and more. We also offer Virtual Office solutions to help your practice where you need the most. Let us know how we can help.
If you are interested in learning more about our billing services, optimization tools or add-on solutions, feel free to reach out to us on our website or via email at businessdevelopment@hpiinc.com
Subscribe to our Health Prime blog to stay tuned on our upcoming webinars and all the latest updates to optimize your medical practice so you can focus on what matters the most: your patients.





-3.png)
-3.png?width=380&name=health-prime-logo5%20(002)-3.png)
Submit a Comment